Lin, K.M, James, E.W., Spitze, E. & Fabricant, P.D. (2018). Pediatric and adolescent anterior shoulder instability: Clinical management of first-time dislocators. Current opinion in pediatrics, 30, 49-56. doi: 10.1097/MOP.0000000000000566.
The Skinny:
- Shoulder instability for pediatric and adolescent patients is fairly common and is often complicated by a high re-dislocation rate. Shoulder instability typically occurs after an acute traumatic event or cumulative repetitive microtrauma (such as baseball pitching) and can be further aggravated by pediatric joint hypermobility. Shoulder instability can occur in many planes of movement: anterior, posterior, or multi-planar however, anterior dislocation and subsequent instability is most common.
- This purpose of this study is to analyze the outcomes of conservative versus surgical management of anterior instability in pediatric and adolescent patients in light of the recent trend towards early surgical stabilization.
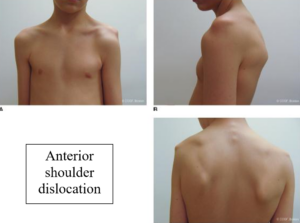
In the Weeds:
- Studies have shown that hypermobility shoulder dislocation per 100,000 people is 0.92 for children ages 0-9 years old, 39.71 for adolescents ages 10-19 years old, and 23.9 for overall ages. This data indicates that shoulder instability after initial dislocation most frequently occurs in adolescents.
- Two factors have been connected with the high recurrence rate of shoulder instability for adolescents. The most dominant being retained collagen elasticity after childhood. Additionally, the authors theorize that patients with closed growth plates are more likely to have a recurrent dislocation (88%) than those with open growth plates (53%).
- These findings assert that children tend to have significantly less recurrence of dislocation than adolescents overall and therefore surgical intervention for younger patients may be unnecessary and may predispose them to undue risk of surgery complications.
- The article further suggests that patients under 25 years of age are likely to have recurrent instability regardless of intervention. These patients have a non-operative recurrent instability rate as high as 90% after an initial dislocation without intervention, and recurrent instability rates after surgery linger around 20%.
Bringing It Home:
- Currently, therapy remains the final form of treatment for 60% of patients under 25-years-of-age. Early implementation of therapy focusing on scapular and rotator cuff strengthening has demonstrated the best outcomes to reduce incidence of recurrent instability. Four to five weeks of therapy following initial dislocation allows pediatric and adolescent patients to regain full motion and strength and decrease apprehension with use.
- Without intervention and strengthening post-dislocation, recurrent instability can cause persistent symptoms that effect quality of life, and lead to chondral damage in the shoulder, placing the patient at risk for developing symptomatic osteoarthritis.
- Limitations: The article does not mention the statistical improvements for patients with recurrent instability who participate in therapy versus those patients who do not complete therapy or undergo surgery.
2 Comments
Leave a Comment
More To Read
Shoulder Pain: The Effectiveness of Conservative Treatment
Reference: Steuri, R., Sattelmayer, M., Elsig, S., Kolly, C., Tal, A., Taeymans, J., & Hilfiker, R. (2017). Effectiveness of conservative interventions including exercise, manual therapy and medical management in adults with shoulder impingement: a systematic review and meta-analysis of RCTs. British journal of sports medicine, 51(18), 1340–1347. https://doi.org/10.1136/bjsports-2016-096515 By: Tayler Roost The Skinny: This study…
The Use of Neuromuscular Electrical Stimulation with Upper Extremity Paralysis
The Use of Neuromuscular Electrical Stimulation with Upper Extremity Paralysis By: Mikayla Murphy Martin, R., Johnston, K., & Sadowsky, C. (2012). Neuromuscular electrical stimulation–assisted grasp training and restoration of function in the tetraplegic hand: A case series. The American Journal of Occupational Therapy, 66(4), 471-477. https://doi.org/10.5014/ajot.2012.003004 The Skinny The purpose of the study was to…
Does mirror therapy work for hand therapy patients with general orthopedic conditions?
By: Maddie Mott Rostami, R. H., Arefi, A., & Tabatabaei, S. (2013). Effect of mirror therapy on hand function in patients with hand orthopaedic injuries: a randomized controlled trial. Disability and Rehabilitation, 35(19). 1647-1651. DOI: 10.3109/09638288.2012.751132 The Skinny: How does mirror therapy work? Mirror therapy (MT) is performed by placing the patient’s injured extremity into…
Hand Therapy: How to Treat the Client with a New Distal Radius Fracture
A short blog post on the basics of treating a Distal Radius Fracture.
Sign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.





good information, I get young adults with shoulder dislocations and many times when I ask if this had happened before it’s like they think I have a crystal ball into their younger days. They say How do you know?
That is funny! Thanks for sharing. Miranda