Teo, S. H., Ng D. C., Wong, Y.K.(2018). Effectiveness of proximal interphalangeal joint blocking orthosis vs metacarpophalangeal joint blocking orthosis in trigger digit: A randomized clinical trial. Journal of Hand Therapy, 1-7.
The Skinny- This study compared PIP joint immobilization via an Oval-8TM with a custom MCP blocking orthosis in the treatment of trigger finger.
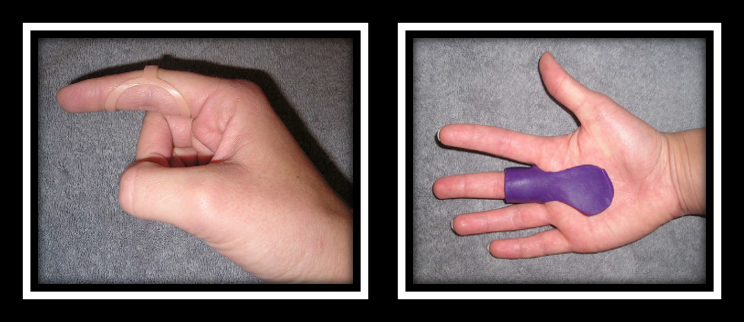
In the Weeds – Patient (n=35) with Trigger Finger (n=43) were analyzed. Twenty-three patients were allocated to the PIP joint splinting group and 20 patients were in the MCP splinting group. Patients wore the orthosis for eight weeks.
Pain reduction was observed in both groups, but pain reduction was greater with PIP joint splinting compared to the MCP joint splinting group (MCP joint splint). There was only significant improvement in QuickDASH for the PIP splinting Group. Patients wore the pip joint splint significantly longer during the day compared to the MCP splinting group (MCP splint), most likely due to improved comfort.
Bringing it Home- Findings suggest both orthoses are effective in reducing QuickDASH scores, reducing pain and improving overall trigger finger symptoms based on Green’s Classification. However, the pip joint immobilization splint was better for improved function and improved compliance.
The rationale for the rating. Small sample size. All patients with comorbidities were excluded limiting the generalizability of findings. Immobilizing the PIP joint compared to the MCP allows more function and improved compliance. When immobilizing the MCP you limit intrinsic grasp which is a necessity for function. The authors recommend wearing the orthosis for a 4-week duration of 24 hours in order to reduce triggering symptoms followed by night-time splint wear for another 3-4 weeks.
4 Comments
Leave a Comment
More To Read
Therapeutic Exercise vs Therapeutic Activity
What is the difference between therapeutic exercise vs therapeutic activity? Therapeutic exercise is billed as 97110 and Therapeutic activity is billed as 97530. Both are CPT codes that are commonly used in occupational and physical therapy billing. These codes are very similar and are often confused. So, when and what do you document for each…
How Weather Changes Affect Joint Pain
By: Lucas Godwin How Weather Changes Affect Joint Pain Numerous potential factors can cause weather-related joint pain, including humidity, temperature, precipitation, and changes in barometric pressure. Scientists have performed many studies on joint pain and weather over the years, but so far, none can say for sure what the connection is. Timmermans et al., 2015…
Hand Therapy: Conservative Management of Pediatric Monteggia Fractures
Conservative Management of Pediatric Monteggia Fractures Monteggia fractures in children comprise approximately 2% of pediatric elbow fractures and involve a fracture of the proximal ulna with dislocation of the radial head (Fig. 1). The primary concern of Monteggia fractures includes the treatment (monteggia fracture treatment pediatric) and relocation of the radial head, because if left…
Early Mobilization After Volar Locking Plate Osteosynthesis of Distal Radius Fractures in Older Patients: A Randomized Controlled Trial
By: Rachel Reed Sørensen, T. J., Ohrt-Nissen, S., Ardensø, K. V., Laier, G. H., & Mallet, S. K. (2020). Early Mobilization After Volar Locking Plate Osteosynthesis of Distal Radial Fractures in Older Patients-A Randomized Controlled Trial. The Journal of hand surgery, S0363-5023(20)30276-8. Advance online publication. https://doi.org/10.1016/j.jhsa.2020.05.009 The Skinny: The purpose of this randomized controlled trial was…
Sign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.






Trigger finger is easy to fix with surgery release. I’ve had it done. Piece of cake.
Have seen a pt lose a finger due to a freak release surgery accident. Have seen the scar tissue left behind following a surgical release replicate a trigger digit. Have seen conservative management effectively treat a trigger digit.
Even simple surgeries carry risks for pts, especially if there are preexisting conditions like diabetes or Raynaud’s. So maybe it is best to explore all aspects of treatment before throwing out a blanket statement, right?
why go to surgery before all conservative measures? Before surgery I would certainly consider CSI, which most times resolve the situation. another thing, is inflammation in the body due yo metabolic issues also need to be considered
What are some suggestions for pediatric trigger finger in the thumb?