Effectiveness of Conservative Therapy and Splinting for 1st CMC OA
Filed under Treatments
Tsehaie, J., Sprekraijse, K., Wouters, R., Slijper, H., Feitz, R., Hovious, S., & Selles, R. (2018). Outcome of a Hand Orthosis and Hand Therapy for Carpometacarpal Osteoarthritis in Daily Practice: A Prospective Cohort Study. American Society for Surgery of the Hand, 1-11.
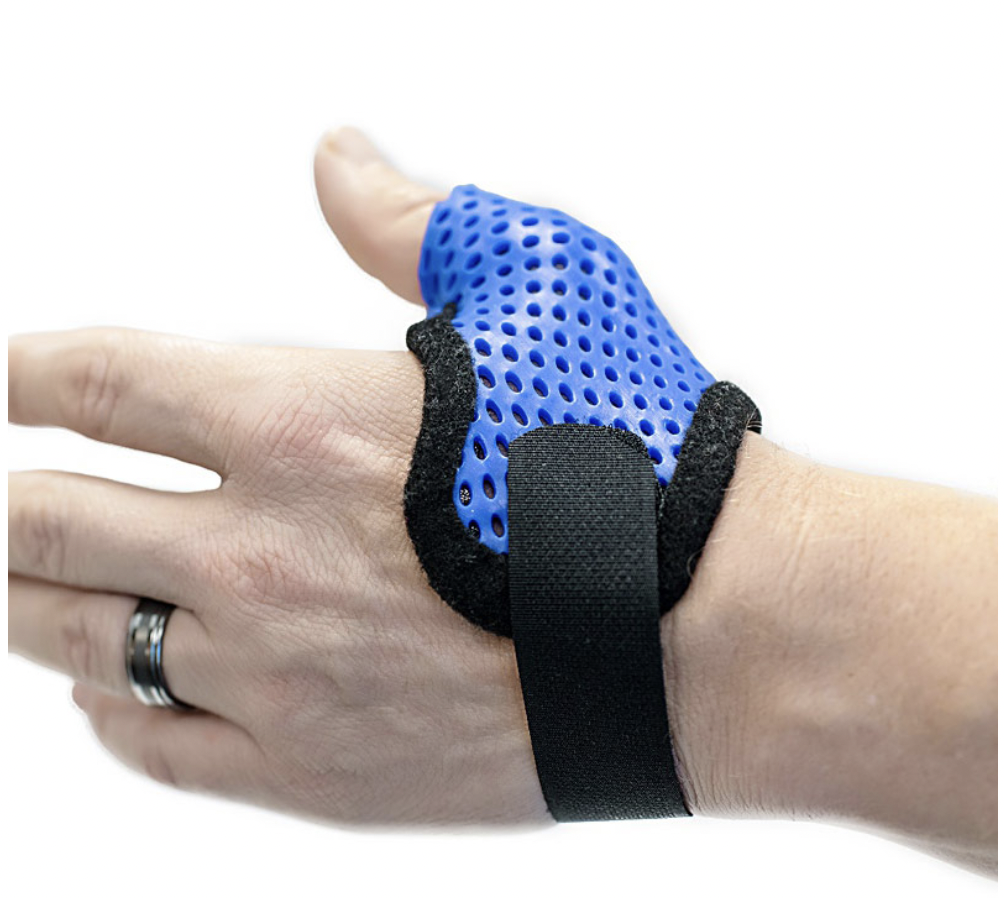
The skinny: Non-surgical approaches (hand therapy & orthotics) are typically the go-to for 1st CMC osteoarthritis. However, there isn’t much solid evidence regarding the efficiency of this approach. And some individuals end up getting surgery despite receiving non-surgical approaches. The primary objective of this prospective cohort study was to determine how just effective hand therapy and immobilization orthotics actually are for CMC osteoarthritis.
With a large sample size, a 12-month intervention, and an extended follow-up period, this article investigated whether non-surgical interventions should occur prior to those that are surgical. Orthotic use and regular hand therapy were proven to reduce pain and increase function in this study.
In the Weeds: In this study, Tsehaie, et al. (2018) describe the results of 809 individuals with CMC arthritis who engaged in hand therapy and orthotic use across 11 locations in the Netherlands. Researchers used this study to describe the efficiency of non-surgical hand therapy and orthotics as well as the rate of conversion from non-surgical to surgical approaches in this population.
Participants who met inclusion criteria were evaluated at an outpatient hand therapy clinic and diagnosed with CMC OA between the years of 2011-2014. Only 122 of the 809 participants completed all follow-up measures. However, surgical data were available for all 809-individuals.
Phase 1 of this study (week 0-6) included instructions for CMC orthosis to be worn 24-hours per day with hand therapy sessions that emphasized thumb positioning and range of motion.
Phase 2 of this study (week 7-12) began to phase out orthotic use as was appropriate based on reports of pain as well as CMC stability. During phase 2, hand therapy sessions also began to be phased out, with more of an emphasis placed on home exercises programs.
Outcome measures for this study were recorded at baseline, 6-weeks, 3-months, and at 12-months. These measures included the visual analog scale for pain and the Michigan Hand Questionnaire for a self-report of function. On top of these outcomes, each participant had a follow-up appointment with their hand surgeon after 3-months to determine whether surgery for their CMC OA was recommended.
124 out of the 809 individuals in this study were identified to have had surgery for their CMC OA.
Pain: Pain was observed to significantly decrease after the 12-month non-surgical intervention for CMC OA. It should be noted that most of that progress, however, occurred during the first 6-weeks.
For individuals who had severe pain going into the study, significant pain reduction was reported. However, for those who didn’t have much pain going in, there was actually an increase in pain. This may have been due to increased awareness due to the intervention.
Function: Function improved significantly after 6-weeks for individuals in this study. Unfortunately, however, that significance was not maintained when it was measured again at 12-weeks.
Bringing it Home:
After an average follow-up of 2.2 years, only 15% of individuals who had received non-surgical interventions for CMC osteoarthritis were converted to surgical treatment. Of those who did not have surgery, non-surgical interventions showed significant reduction in pain as well as improvements in function.
In line with previous evidence, most of this pain reduction was observed to occur in the first six weeks of treatment; and then maintained after that. Keep in mind that during that first 6-weeks, orthoses were worn all day, every day.
Individuals who reported ‘more’ pain and ‘less’ function at the start of the study, were slightly more likely to end up in the operating room. However, for those that did not receive surgery but did have high pain levels initially, the most significant pain reductions post-intervention were seen.
Rating: 4 out of 5 stars.
The strengths of this study included a large sample size as well as a natural setting. Unfortunately, the ‘natural’ setting also brought weaknesses along with it; including non-compliance, increased drop-out rates, and inconsistencies between treatment sessions.
Despite the mentioned weaknesses, we think that the researchers did a good job with this one. The study supports hand therapy as an initial treatment for CMC osteoarthritis and should provide confidence to you hand therapists out there striving to provide the best possible care for your clients.
1 Comments
Leave a Comment
More To Read
Taping and Thumb Arthritis: Rapid Review
Hugo, J., and Valdez, K. Mobilization with movement and elastic tape application for the conservative management of carpometacarpal joint osteoarthritis. Journal of Hand Therapy, 28, 2015; 82-85 Practice Forum The Skinny: The authors demonstrated a useful technique for mobilizing the thumb CMC joint followed by the application of k-tape (kt tape thumb arthritis). In the…
Read MoreGraded Motor Imagery in Hand Therapy
The 3 Stages of Graded Motor Imagery We’ve all heard of mirror box therapy, but do you know the details of how it works? There’s actually 3 stages involved that exercise the brain and take advantage of its plasticity. There is a great deal of evidence supporting these three stages and you can use them…
Read MoreComparing IP and MCP joint splinting for Trigger Finger
Teo, S. H., Ng D. C., Wong, Y.K.(2018). Effectiveness of proximal interphalangeal joint blocking orthosis vs metacarpophalangeal joint blocking orthosis in trigger digit: A randomized clinical trial. Journal of Hand Therapy, 1-7. The Skinny- This study compared PIP joint immobilization via an Oval-8TM with a custom MCP blocking orthosis in the treatment of trigger finger. …
Read MoreSign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.





Very nice work. Thanks