CMC Arthritis Orthosis in the Hand: Mechanics and Purpose
Filed under Orthoses
One of the most common diagnoses we see in hand therapy is osteoarthritis of the 1st carpo-metacarpal joint where the metacarpal articulates with the trapezium. Also known as basal joint arthritis (CMC arthritis), this causes pain, joint deformity, loss of strength and loss of function. Patients come to us looking for relief of symptoms and a return to function.
In most of these cases an effective treatment strategy is a three-pronged approach:
- Activity modification
- CMC stabilization exercises
- Orthosis use to stabilize the basal joint.
For now, I want to focus on the CMC orthosis for basal joint arthritis and how it works to stabilize, protect and aid in grasp and functional hand use. To understand this, we first need to understand how osteoarthritis affects the thumb.
How Osteoarthritis Affects the Thumb
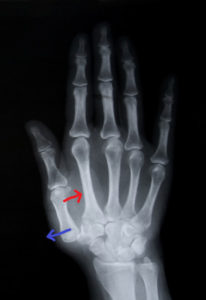
As cartilage breaks down in the saddle joint between the Trapezium and the 1st metacarpal, the joint loses internal stability. This creates pain with bone-on-bone friction. The ligaments also are now too laxed with the void left by the cartilage. This allows the metacarpo-phalangeal joint to radially sublux (Blue Arrows) out of position during pincer or power grasp usage. This happens when the Adductor Pollicis contracts (Red Arrows) and pulls the distal head of the metacarpal ulnarly.
Without the stability of taught ligaments to maintain approximation of the CMC joint, the proximal end cantilevers radially, away from the joint. This results in subluxation that can become a chronic position, called a ‘shoulder sign’ (shoulder sign thumb).
As the CMC joint subluxation worsens, the system tries to correct by stabilizing the 1st metacarpal against the second metacarpal with adduction. Unfortunately, this causes 2 negative outcomes:
- Further radial cantilever of the proximal head
- Tightening of the AP into a contracted position.
This subluxation pattern becomes more pronounced, painful and limiting to functional use. Without correction, this will continue to degrade the stability of the joint.
How CMC Orthosis Can Protect Against Joint Damage in the Hand
This is where orthosis use can be helpful in slowing this progression and protecting against further joint damage. A CMC short opponens orthosis is designed to protect the basal joint’s stability during grasp as well as helping maintain a functional opposition/abduction position at rest without furthering the subluxation.
Here are two primary ways orthosis can help protect from damage:
1. Maintain Approximation
The first mechanism of the short opponens splint is to maintain approximation of the CMC joint. Unlike other orthoses, this splint does not need to cross the joint to be effective. With simple radial support to the proximal metacarpal head the joint is approximated as the ulnar strap helps maintain contact and stability.
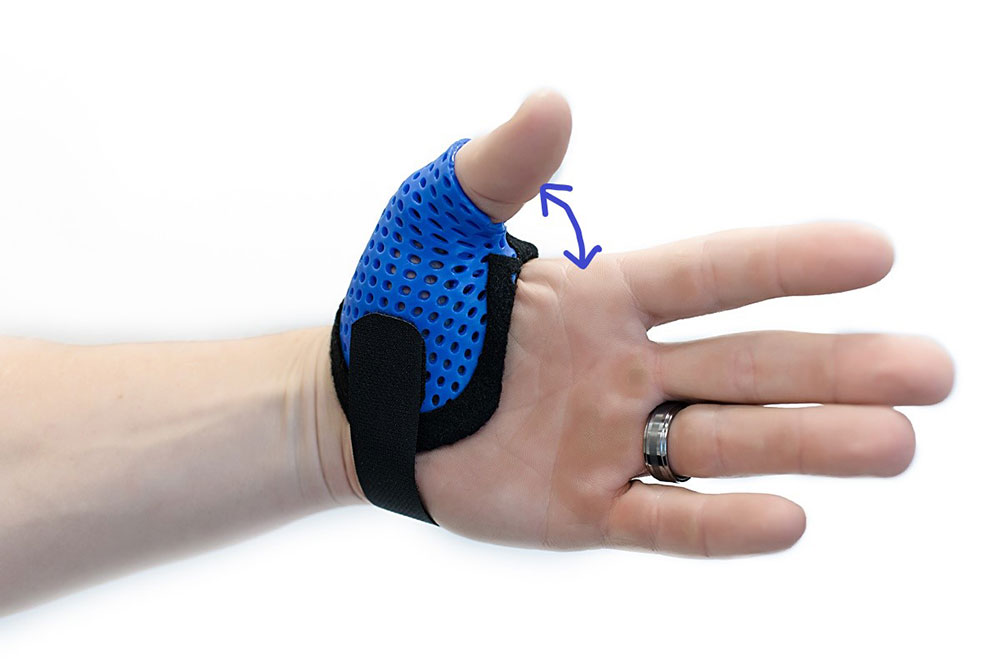
2. Maintain the Web Space
Second, the splint maintains the web space in a functional position with abduction and slight opposition. This is a better functional position for use without pain, but it also allows the AP to relax and lengthen. Decreased tension in the AP reduces the cantilever subluxation to the CMC joint.
3. Provide Mechanical Support
Finally, the stability of the thermoplastic around the CMC joint provides mechanical support during pincer and grip activities. For every 1 lb of force applied at the tips of a pincer grasp there is 12 lbs of force applied to the CMC joint. Using a Short Opponens orthosis provides an external support that the arthritic thumb lacks internally. The solid backing around the CMC prevents subluxation and shift during grip activities and pincer grasp.
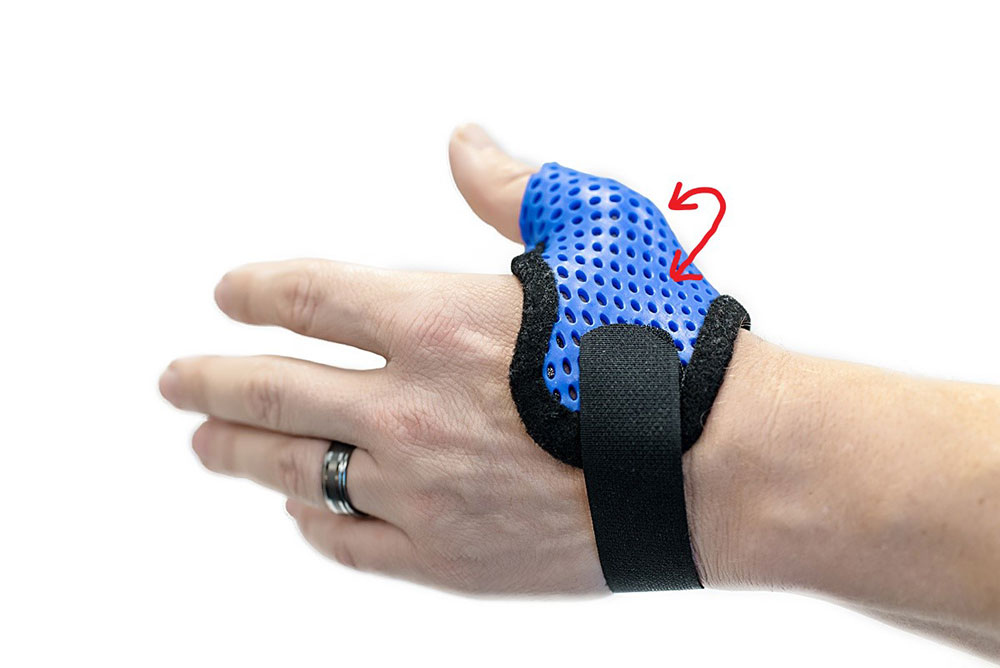
The use of a short opponens orthosis provides light approximation of the CMC joint, improves functional grasp position for decreased AP tension and mechanical support to augment laxity in the joint capsule.
While use of an orthosis is only one aspect of treatment planning for basal joint osteoarthritis, it is a crucial aspect to improving the quality of life for the patient. If you want to see two options for how to make this important orthosis, check out our video with explanation on a version with and without a template.
23 Comments
Leave a Comment
More To Read
6 of our Favorite Adaptive Equipment Tools for CMC Osteoarthritis
Individuals struggling with osteoarthritis of the 1st CMC joint usually have difficulty with daily activities and it can become very frustrating. Everyday tasks such as cutting food, opening containers, and donning a button up shirt can become painful and slow. The largest contributor to the overall function of our hand is the thumb. If the…
The Influence of Psychological Factors on Outcomes Following Wrist and Hand Injuries: A Systematic Review
The Influence of Psychological Factors on Outcomes Following Wrist and Hand Injuries: A Systematic ReviewArticle: Minnucci, S., Fochi, F., Lerose, E., Scalise, V., & Brindisino, F. (2025). The influence ofpsychological factors on outcomes following wrist and hand musculoskeletal injuries: Asystematic review. Journal of Hand Therapy. https://doi.org/10.1016/j.jht.2025.10.005 The Skinny:Wrist and hand injuries are common worldwide and…
Hand Therapy as a New Grad or Student
Tips for Getting Prepared for hand therapy as a new grad or a Level II Fieldwork Everything you need to know in hand therapy starts with the upper extremity anatomy. Here is a quick checklist to review and hopefully help get you started in your new hand therapy setting. By: Tristany Hightower I suggest, as…
What is Chronic Exertional Compartment Syndrome? Overview and Hand Therapy Treatment Ideas
Compartment syndrome is a condition characterized by increased pressure within a compartment of the body, leading to pain, swelling, and reduced tissue perfusion (Barkay et al., 2021; Buerba et al., 2019). It can be either acute or chronic (Barkay et al., 2021). Chronic exertional compartment syndrome (CECS) is a rare type, most commonly observed in…
Sign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.






Well done Josh! Perfectly worded!!!
Thanks!
This is a very helpful explanation of CMC Arthritis! What is the recommended splint wearing schedule (Night/day, duration, etc.)? Thank you!
I recommend wearing when active. It isn’t needed when sleeping or when at rest (e.g. watching T.V.). But wearing it as often as possible during any level of activity will relieve pain and protect the joint.
Josh, It is very benefit explanations for CMC Arthritis well done Thanks. PT. Firdevs
I’m glad you found it helpful.
Where can I buy one of these?
Clinical Pearl
When making a spica: Just after you placed the material on the patients hand place a small rubber bouncy ball between the index finger and thumb.
This correctly aligns the thumb and allows you to see where you may need to trim.
Patients find this method much more comfortable
Well written and great info for OT who does not see hands all the time.
Even long time practicing hand therapist can learn from articles like this I never would’ve thought to put a small bouncy ball in between the thumb and the index. Perfect idea
Thanks for commenting!! It is so fun being a part of a community that has a culture of sharing.
Thank you!
I am very petite & need one of these! I’m an active OT. I have been using elastic tape cut in half lengthwise and making my own but with COVID, that splint would be so much nicer!
I appreciate any assistance!
alwaysoccipied@live.com
Thank you
The elastic tape is an excellent idea. A custom splint works well or you could try try the Metagrip push splints as well. They are low profile and aren’t as restrictive for work
Hello dear Miranda,
a great article and a great orthosis, what is the cut plan? ICh am from Germany and an enthusiastic reading hand therapist.
Greetings
Kathrin
I would love to see a pattern for the orthosis if you have it available. Or even a quick tutorial on how to make. I make thumb spica’s different than this but this is less cumbersome and in the palmar surface. Thanks for all the good information.
Hi Krista !
If you go to our IG page @handtherapyacademy we provide tutorial on orthosis fabrication for free. If you want a more detailed explanation we have a monthly membership.;
Miranda
I like the way you described this. Thanks.
Hi thank you for the wealth of information.
I did recently see an orthopedist for my new cmc arthritis in both thumbs. He prescribed analgesics and a CMC joint splint- fairly large I might add.
Question- yours is so much different looking than the one he prescribed but I might be willing to try it if I knew where to get it.
Also, it’s unclear to me how often I wear the brace. I was told if I’m doing an activity involving my thumb where I experience more pain I would wear it but warned against wearing it all the time because arthritis needs movement. Thank you!
Hi Barb, Head over to HTCC.org and look for a local CHT in your area. They can help you with a splint and when to wear it.
Hello,
What is the black material used on the edge of the splint? This would be very helpful at my clinic. We usually smooth the edges, but this can still be uncomfortable for certain splints.
Thanks!
it is a black felt edging we order from SME, which is a medical supplier for therapy.
it felt splint edging we order it from SME medical. which is a therapy equipment supplier.