How many of us have practiced suture removal in occupational or physical therapy school?? NOT I!!

Often, hand surgeons will ask the therapist to remove sutures and sometimes the order will even say “remove sutures when ready”
SO NOW WHAT? How to remove continuous sutures? First, we can cover the basics of sutures!
There are two basic classifications for suture material, absorbable and non-absorbable. Absorbable sutures typically do not require manual removal, because the enzymes that live in the body’s tissue will digest them. Non-absorbable require a healthcare practitioner to remove them however sometimes they can be left in permanently for example sutures placed in tendons are typically never removed.
You may encounter patients with different types of sutures, or a different technique was utilized to place them.
The most common types of suture techniques you will see in the hand therapy setting is the interrupted suture techniques followed by the continuous sutures.
Interrupted Sutures:
After a stitch is made the material is cut and tied together. After this another stitch is placed and again cut and tied together, this step is typically repeated until the wound is closed. This technique usually takes a little longer than the continuous suture removal technique.
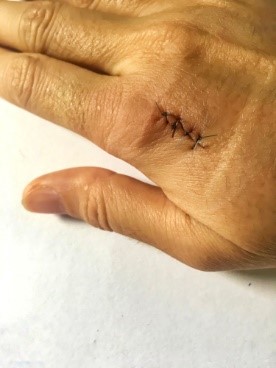
Continuous Sutures:
A series of stitches that use one single strand. This allows the tension to be distributed evenly. These are typically very easy to remove and can be placed quickly.
Buried Sutures: This is when the knot of the suture is found within the tissue. This suture is typically not removed.
Deep Sutures: These are placed in the layers of the skin and deeper tissues. These are either continuous or interrupted. Typically, these are used to close fascial layers.
Now for the Million Dollar Question? When should the sutures be removed?
This often will vary form patient to patient and may be dependent on how well the wound is healing. If the patient is diabetic and demonstrating poor wound healing or poor wound closure you may be inclined to leave the sutures in place a little longer compared the young kid whose incision is healing very well.
Guidelines for Suture Removal
Arms 7-10 days
Dorsal aspect of the Hand 10-14 days
Palms of Hand 14-21 days
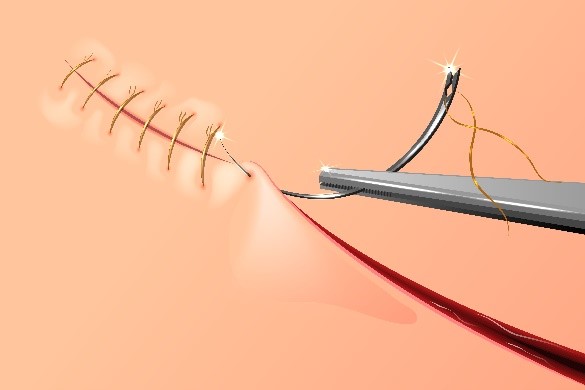
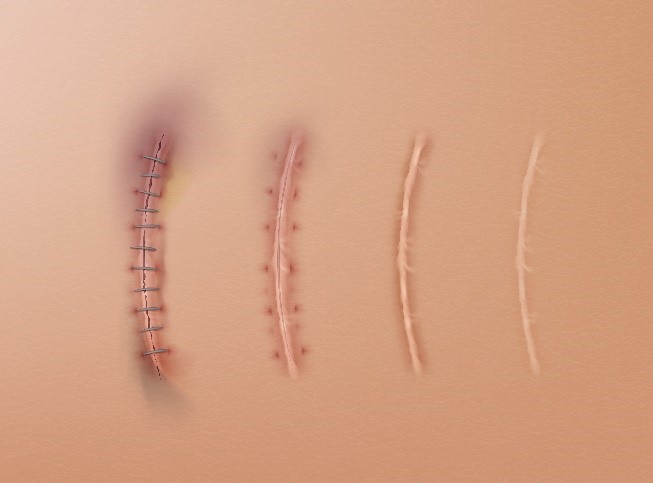
When removing the sutures make sure you use a sterile suture removal kit. Pick up one end the suture and cut it, trying to stay as close to the skin as possible. After it is cut slowly pull the suture strand.
1 Comment
Leave a Comment
More To Read
Soft Tissue Healing in Pediatrics
By: Chelsea Gonzalez Why do pediatric clients often not require as much hand therapy for soft tissue injuries when compared to adults? The simple answer: Kids have very elastic soft tissue, which can return to its original shape and position after stretch. This elasticity is lost with time as collagen fibers expand and their internal…
Surgery & Hand Therapy Highlights for Dupuytren’s Disease
Dupuytren’s disease affects the fascia of the hand (Dupuytren’s fasciectomy hand). It is relatively common to encounter patients with Dupuytren’s condition, even if that is not the primary reason you are treating the patient. Patients often present with a nodule(s) in the palm of the hand, or they may even have a thickened cord running…
Title: Understanding De Quervain’s Pathology: A Comprehensive Exploration of Special Tests
Understanding De Quervain’s Pathology: A Comprehensive Exploration of Special Tests By: Miranda Materi De Quervain’s and Special Tests De Quervain’s tenosynovitis is a condition characterized by inflammation of the tendons on the thumb side of the wrist, causing pain and discomfort. These tendons include Abductor Pollicis Longus (APL) and Extensor Pollicis Brevis as they pass through…
Therapeutic Exercise vs Therapeutic Activity
What is the difference between therapeutic exercise vs therapeutic activity? Therapeutic exercise is billed as 97110 and Therapeutic activity is billed as 97530. Both are CPT codes that are commonly used in occupational and physical therapy billing. These codes are very similar and are often confused. So, when and what do you document for each…
Sign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.






Yourwebhoster.eu