Surgical vs. Conservative Treatment for Pediatric Trigger Finger
Filed under Uncategorized
Jia, L., King, J. D., Goubeaux, C., Belardo, Z. E., Little, K. J., Samora, J. B., Marks, J., &
Shah, A. S. (2023). Presentation and management of the pediatric trigger finger: A
multicenter retrospective cohort study. The Journal of Hand Surgery, 48(7), 665–672.
https://doi.org/10.1016/j.jhsa.2023.03.015
Article Review: Kelsy Melton

The Skinny: The goal of this study conducted by King et al., (2023) was to compare operative
and nonoperative treatment outcomes for pediatric trigger finger (PTF) based on presentation of the
condition. This is a rare and under-studied condition that can come from several anatomical
etiologies including the thickening of flexor digitorium profundus (FDP) and/or flexor digitorum superficialis (FDS), or an abnormal relationship between FDS or FDP, or constriction of the A1, A2 or A3 pulleys.
This was a retrospective cohort study conducted through the medical record review of three children’s
hospitals. The record review identified patient demographics, pediatric trigger finger characteristics, treatment strategies, and outcomes and ultimately included 321 patients 18 years and younger with a
combined total of 449 PTFs.
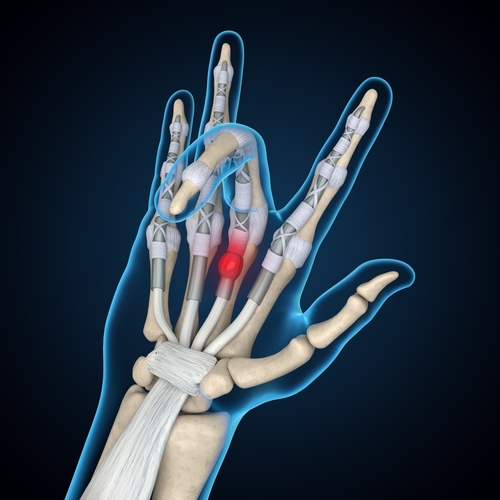
In the Weeds: Patients were excluded from the study if they had prior surgeries on the affected
digits or if they had a predisposing medical condition. Medical record reviews included patient
and pediatric trigger finger characteristics, nonsurgical treatment strategies, duration, and outcome, as well as operative treatment strategies, complications, and outcomes. Nonsurgical treatment strategies
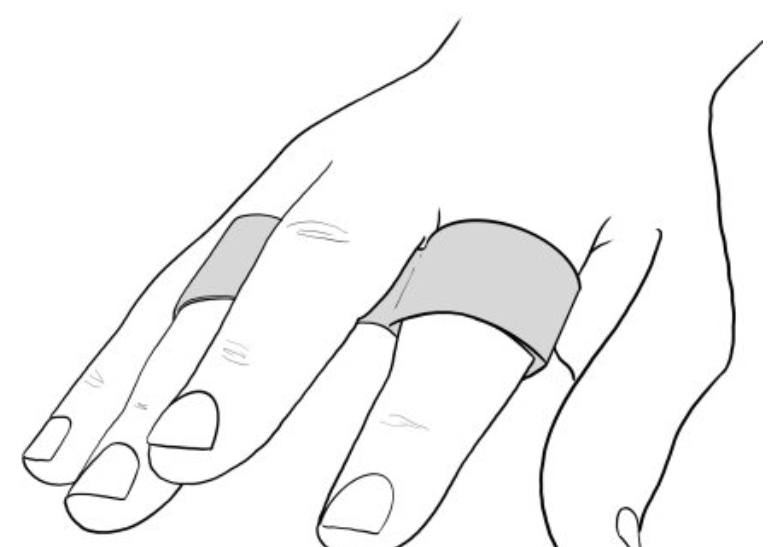
included monitoring, stretching, nighttime extension splinting, nonsteroidal anti-inflammatory
drugs, and corticosteroid injections. Operative treatment included A1, 2 and/or 3 pulley release,
ulnar and radial FDS slip excision, and mass/tumor removal. A statistical analysis of the reviewed
data was utilized to determine a difference in the resolution of symptoms between splinted vs.
non-splinted pediatric trigger finger. A second analysis was completed to determine the difference between A1 pulley release alone versus A1 pulley release in combination with other procedures.
Bringing it Home: 80% of patients pursued non-surgical management of pediatric trigger finger initially, but after persistent worsening of symptoms 20% of those patients sought surgical intervention. The most common nonsurgical management was extension splinting and monitoring, resulting in 75% of
these pediatric trigger fingers achieved complete resolution of symptoms within 6 months., but high-grade pediatric trigger figners were significantly less likely to achieve this complete resolution with non-surgical management.
Overall, it was found that pediatric trigger fingers managed operatively had significantly higher rates of complete resolution compared with those managed conservatively. This confirmed the authors’ hypothesis that operatively managed pediatric trigger fingers have a significantly higher rate of symptom resolution than conservatively managed pediatric trigger fingers.
Rating: Overall, this study receives a 3 out of 5 rating. The large sample size and significant
findings of this study provide valuable insight into the treatment of a historically under-studied
condition. One of the biggest limitations of the study involves the potential for bias due to it
being a retrospective review. It is also possible that these findings are not generalizable to
patients with a predisposing medical condition, since these individuals were excluded from the
study.
More To Read
Dart-throwing Angle in Hand Therapy for Scapholunate (SL) Ligament Injuries.
Does Object Height Affect the Dart Throwing Motion Angle During Seated Activities of Daily Living? Cohen, Y., Portnoy, S., Levanon, Y., Friedman, J. (2020). Does object height affect the dart throwers motion angle during seated activities of daily living. Journal of Motor Behavior, (52) 4. Article Review By: Rita Steffes The Skinny: Dart Throwers Motion…
Read MoreHow To Do A Fast but Thorough Hand Therapy Assessment
We don’t get a lot of time. Sometimes new patients come in unexpectedly or someone comes at the wrong time and your 1-hour block for an eval is suddenly only 30 minutes. Do you know how to get the most out of your eval time with the patient? Do you know what things are the…
Read MoreWhich orthosis design is better for zone 5-6 extensor tendon injuries, a relative motion orthosis compared to a dynamic extension orthosis?
M. Buhler, ˝ D. Gwynne-Jones, M. Chin et al., (2023) Are the outcomes of relative motion extension orthoses noninferior and cost-effective compared with dynamic extension orthoses for management of zones V-VI finger extensor tendon repairs: A randomizedcontrolledtrialJournalofHandTherapy. The Skinny: The aim of this study was to compare the data for two different types of orthoses…
Read MoreSign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.