Differentiating Proximal Median Nerve Entrapment from Carpal Tunnel Syndrome
Filed under Evaluation, Treatments
By: Brittany Day
Proximal Median Nerve Entrapment, Pronator Syndrome, or Lacertus Syndrome?
Pronator syndrome is a term used to describe proximal median nerve entrapment (PMNE) in the forearm. Pronator syndrome and lacertus syndrome are sometimes used interchangeably to describe proximal median nerve entrapment distal to the ligament of Struthers and proximal to the flexor superficialis arch on the medial side of the forearm (lacertus syndrome vs pronator syndrome). While there is some distinction between the exact location of the compression; the testing, symptoms, and interventions remain similar. The majority of PMNE occur at the level of the lacertus fibrosis sitting superficially to the pronator muscle on the medial aspect of the proximal forearm. Level of compression, provocative testing, symptomology, and interventions of PMNE differ from carpal tunnel syndrome (CTS) and are discussed below.
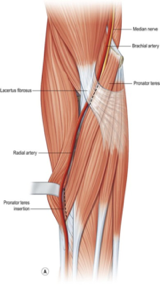
A Diagnostic Conundrum
This illusive syndrome is difficult to diagnose with a need for objective measures as seen through the lens of evidence-based practice. Current diagnostic procedures for PMNE are mostly from subjective clinical findings such as patient self-report and provocative testing. Unlike CTS, a compression at the PMNE will likely not cause the axonal damage found with NCV or EMG. These objective measures generally come back negative for median nerve compression and have a specificity between 30%-70%. MRI results will also likely come back negative for PMNE. A prospective study of 44 participants with PMNE used (1) weakness in median innervated muscles distal to the lacertus fibrosus, (2) pain with palpation over the median nerve at the level of the lacertus fibrosus, and (3) a positive scratch collapse provocative test, as diagnostic criteria.
Signs and Symptoms
Signs and symptoms of PMNE at any level differ from that of CTS and will likely include:
- Loss of lateral pinch and tip pinch strength
- Loss of fine motor skills
- Weakness of FPL, Digit 3 FDP, and FCR found with manual muscle testing
- Pain with palpation of median nerve at the level of the lacertus fibrosis (also known as the bicipital aponeurosis).
- Positive scratch collapse test at level of the lacertus fibrosis
- Pain that likely does not increase at night (a hallmark symptom of CTS)
How to Complete the Scratch Collapse Test for PMNE
- Have patient seated in a chair with feet on the ground, wrists in neutral, and elbows at 90 degrees of flexion
- Patient to resist internal rotation with external force given bilaterally
- Scratch the uninvolved anterior forearm at the level of the lacertus fibrosis and provided external force for patient to resist bilaterally
- Scratch the involved anterior forearm at the level of the lacertus fibrosis and provide external force for patient to resist bilaterally
- A positive test will result in patient “collapsing” into internal rotation with external force
Common PMNE Treatments (lacertus syndrome treatment)
- Non-invasive Treatment – Rest, splinting, and NSAIDs for 3 months
- Injection Treatment – Ultrasound guided perineural injection of median nerve at level of lacertus fibrosis
- Surgical Treatment – Surgical decompression of median nerve with release of lacertus fibrosis
References:
Delzell, Patricia B, & Patel, Mital. (2019). Ultrasound‐Guided Perineural Injection for Pronator Syndrome Caused by Median Nerve Entrapment. Journal of Ultrasound in Medicine, 39(5), 1023-1029.
Hagert E. (2013). Clinical diagnosis and wide-awake surgical treatment of proximal median nerve entrapment at the elbow: a prospective study. Hand (New York, N.Y.), 8(1), 41–46. https://doi.org/10.1007/s11552-012-9483-4
Lalonde, D. (2015). Lacertus syndrome: A commonly missed and misdiagnosed median nerve entrapment syndrome. BMC Proceedings, 9(S3), A74.
3 Comments
Leave a Comment
More To Read
Does Taking an Alpha-lipoic for 40 days after Carpal Tunnel Release decrease the likelihood of developing Pillar Pain?
Filippo, B., Granchi, D., Roatti, G., Merlini, L., Sabattini, T., & Baldini, N. (2017). Alpha-lipoic acid after median nerve decompression at the carpal tunnel: A randomized controlled trial. The Journal of Hand Surgery, 4, 236–42. The Skinny – A double-blind, randomized controlled study was performed. Sixty-four patients were randomly assigned into two groups after median…
Read MoreSoft Tissue Healing in Pediatrics
By: Chelsea Gonzalez Why do pediatric clients often not require as much hand therapy for soft tissue injuries when compared to adults? The simple answer: Kids have very elastic soft tissue, which can return to its original shape and position after stretch. This elasticity is lost with time as collagen fibers expand and their internal…
Read MoreCarpal Fractures: A Brief Overview
Carpal fractures account for 8% of fractures in the upper extremity. The carpals are situated between the (distal radius and ulna) and the metacarpals. They make up the proximal row- Scaphoid, Lunate, Triquetrum, and Pisiform, the distal row- Trapezium, Trapezoid, Capitate, and Hamate. Here are some of the most common carpal bone fracture Scaphoid…
Read MoreSign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.




Thanks for info.
very clear and educational
Don’t forget to complete Deep Tissue as tolerated. Many of my baseball players benefit from long flexor and extensor stretch. Be certain to pay attention to the neuroanatomy; you don’t want to get punched in the teeth.