Factors that influence orthosis adherence in patients with acute traumatic tendon injuries to the hand
Filed under Orthoses
Savaş, S., & Aydoğan, Ç. (2020). Factors affecting orthosis adherence after acute traumatic hand tendon repairs: A prospective cohort study. Journal of Hand Therapy, S0894113020301848. https://doi.org/10.1016/j.jht.2020.10.005
World Health Organization. (2003). Adherence to long-term therapies: evidence for action. World Health Organization.
The Skinny
Adherence to orthosis wear is vital for protecting healing tendons after a traumatic tendon injury to the hand to prevent ruptures, deformities, and contractures. This prospective cohort study aimed to analyze the factors that may influence patients’ orthosis adherence after acute traumatic tendon repairs to the flexors or extensors of the hand. This study used the multidimensional adherence model (MAM) published in 2003 by the World Health Organization to assess what factors influence orthosis adherence (Savaş & Aydoğan, 2020). The MAM identifies the five dimensions as influences on adherence include socioeconomic, healthcare system-related, condition-related, treatment-related, and patient-related factors (p.1).
In the Weeds
The study included 133 patients recruited consecutively at an inpatient clinic where their surgeries were performed and where they would receive hand therapy. The study only included participants who had either a flexor or extensor tendon injury to the hand and excluded participants who had any other significant injuries to other structures such as burns, brachial plexus injury (brachial plexus injury orthosis), amputations, fractures, bilateral injuries, tenolysis, history of polyneuropathy, or nerve entrapments or injuries to both flexor and extensor tendons. Participants were also excluded if they had a history of severe psychiatric conditions that impacted cognitive skills.
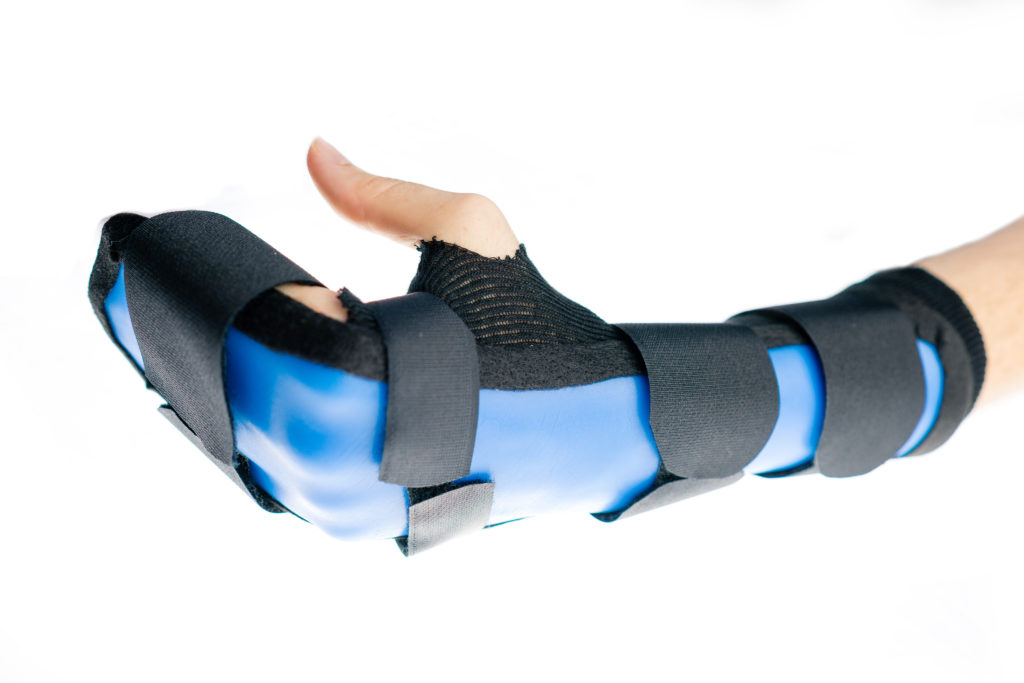
Patients were evaluated three days and three weeks post-operation. On the third day post-op, participants were provided a custom-fabricated orthosis by the same orthotics specialist. Flexor tendon patients received a custom-fabricated forearm-based dorsal blocking orthosis and were prescribed an early controlled passive motion protocol for the following three weeks. Participants with extensor tendon injuries were provided an orthosis based on the zone of injury. Participants with zones 1-2 received DIP immobilizing orthoses, zones 3-4 received PIP immobilizing orthoses, and zones 5-7 received a volar orthosis. All extensor tendon patients were given exercises to do every 4 hours. All participants were given the exact instructions to wear the orthosis 24 hours a day for three weeks, only remove it once a day to wash the hand carefully, and complete all exercises while wearing the orthosis. All patients were educated on the precautions of their injuries and the risk of rupture if they remove the orthosis and use the injured extremity during the four weeks. Each participant was given written instructions and pictures for orthosis wear, precautions, and exercises.
Depression and anxiety were assessed on the first encounter three days post-op using the Beck’s Depression and Anxiety Inventories as an outcome measure for patient-related factors. Socioeconomic factors that were assessed included age, sex, education, marital status, employment, insurance status, monthly income, distance traveled to the hospital, and level of family support. Condition-related factors that were assessed included the cause of injury, nature of the injury, pain at three days post-op, and whether or not it was a work injury. Treatment-related factors included the orthosis type and orthosis-related complaints. Healthcare-related factors assessed included a questionnaire about the participant’s experience with their surgery and postoperative experience, relationship with the surgeon, and satisfaction with the rehabilitation process.
Orthosis adherence was measured at week three post-op. Participants were determined as fully adherent if they reported wearing their orthosis 100% of the time, partially non-adherent if they reported removing their orthosis but did not use their hand, and non-adherent if they reported removing their orthosis and also using their hand. If patients removed their orthosis, they were also asked to specify the frequency and duration of times they removed their orthosis and the reasons for removing the orthosis.
Bringing it Home
This study had an immense amount of outcome measures; for this rapid review, only significant and clinically relevant results from this study will be addressed. Of the 133 participants, 44 (33.1%) patients were fully adherent, 67 (50.4%) were partially non-adherent, and 22 (16.5%) were non-adherent. Seventy-two participants reported removing their orthosis daily. Sixty-six of them reported removing it for less than 15 minutes at a time, seven participants removed their orthosis for 16-30 minutes, and twelve participants removed it for more than an hour at a time. Seven participants had tendon ruptures, and four of them were nonadherent patients. When looking at the reasons for orthosis removal among the partially adherent and non-adherent patients, the number one reason was complaints about the orthosis itself. The complaints about the orthosis included discomfort, soreness, and transpiration (p.7). The second most cited reason for orthosis removal was due to interference with daily activities such as dressing and bathing and the third most cited reason was to complete daily tasks such as housework and personal hygiene tasks.
The correlation between orthosis adherence and person-related factors had significant results regarding depression/depressive symptoms. Depressive symptoms were present in 34.6% of participants, and 17.3% had clinically diagnosed depression. Having higher levels of depressive symptoms at the 3-day post-op assessment was negatively correlated with orthosis adherence. Anxiety, however, did not have any significant effect on orthosis adherence. Treatment-related and healthcare-related factors were not significantly correlated with orthosis adherence in this study.
Rating 3 out of 5
This study had many limitations due to using subjective measures to determine the factors that impact orthosis adherence. The measurement of adherence was also subjective and limits the strength of the results from this study. The authors did identify that there may have been some reporting bias from the participants, and the true adherence rate may be lower than reported. The only truly significant correlation found in this study was that depression at the three-day assessment impacted orthosis adherence by the week three assessment.
Although the evidence was not strong, the data collected in this study can inform how therapists educate their patients on orthosis wear and precautions when working with acute traumatic tendon repairs. This study identified that the most cited reason for removing the orthosis was due to complaints of discomfort and soreness. Therapists can take this into consideration and emphasize to patients that they should report any issues with their orthosis to their therapist or physician so adjustments can be made. This study also identified that participants felt like their orthosis interfered with their ability to perform daily tasks. Therapists can use this information to help patients find solutions to make daily tasks easier while wearing their orthosis during the first encounter to reduce the chance of patients removing their orthosis for those reasons.
More To Read
Hand Therapy Article Review: The Radial Synergy Test, An Aid to Diagnose de Quervain’s Tenosynovitis
Chihua, L., Langford, P.N., Sullivan, G.E., Langford, M.A., Hogan, C.J., & Ruland, R.T. (2021) The radial synergy test: an aid to diagnose de Quervain’s tenosynovitis. HAND. epub ahead of print;1-6. doi: 10.1177/15589447211057297 Rapid Review By: Case Peters The Skinny: de Quervain’s tenosynovitis is a common pathology that involves swelling and thickening of the tendon sheaths…
The effects of cupping therapy as a new approach in the physiotherapeutic management of carpal tunnel syndrome
Article Review By: Rachel Reed Mohammadi, S., Roostayi, M. M., Naimi, S. S., & Baghban, A. A. (2019). The effects of cupping therapy as a new approach in the physiotherapeutic management of carpal tunnel syndrome. Physiotherapy research international : the journal for researchers and clinicians in physical therapy, 24(3), e1770. https://doi.org/10.1002/pri.1770 The Skinny: The purpose of this…
Radial Nerve Palsy: A Paralysis Causing Wrist Drop
Radial Nerve Palsy- Treatment
Changes in ROM of the MCP after Trapeziometacarpal Arthrodesis
Rapid Review: Changes in ROM of the MCP after Trapeziometacarpal Arthrodesis Hayashi, M., Kato, H., Komatsu, M., Yamazaki, H., Uchiyama, S., & Takahashi, J. (2021). Changes in the Functional Range of Motion of the Thumb Metacarpophalangeal Joint After Trapeziometacarpal Arthrodesis for Patients With Advanced Trapeziometacarpal Osteoarthritis. The Journal of hand surgery, S0363-5023(21)00613-4. Advance online publication. https://doi.org/10.1016/j.jhsa.2021.09.018. The Skinny: Several published…
Sign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.